Infection Control In Dental Practice - Introduction
Cleanliness and proper sterilization techniques has been a part of dental practice for many years. However, recently a number of disease causing organisms such as AIDS, hepatitis B and C and herpes viruses have made these techniques even more important.
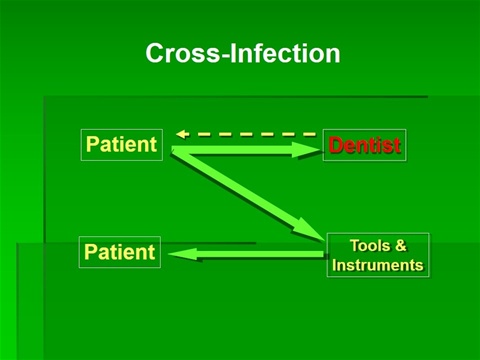
Diseases can be transmitted in dental clinic from patient to patient, from patient to dental health care workers (DHCWs) and to less extent from DHCWs to patients. The unique nature of the dental clinic procedures, instrumentation and patient care settings require a specific strategies regarding the prevention of disease transmission among the DHCWs and their patients.
Dental patients and DHCWs are exposed to variety of pathogenic microorganisms via contact with blood or oral and respiratory secretions. (Table 1)
Table 1. Some organisms that may be transmitted in the dental clinic.
• Cytomegalo-Virus
• Hepatitis B virus (HBV)
• Hepatitis C virus (HCV)
• Herpes simplex virus
• Human immunodeficiency virus (HIV)
• Mycobacterium tuberculosis.
• Staphylococci and streptococci
• Organisms causing upper respiratory tract infection.
Routes Of Disease Transmission
Diseases can be transmitted through direct contact with blood, oral fluids and other secretions. However, the more serious route of disease transmission is through the indirect contact route with the patient material. Contact with contaminated instruments, operatory equipments, environmental surfaces and also contact with air borne contaminants present in either droplet spotter or aerosol of oral and respiratory fluids are all possible sources for indirect disease transmission.
Most of the DHCWs are well aware about the direct contact route of disease transmission. The problem, however, is in the indirect route.
Sterilization And Disinfection
Sterilization can be defined as the process by which all the microorganisms are eliminated from a surface of an instrument. Sterilization is a process of yse or no. Nothing can be half sterilized.
Disinfection, on the other hand, is the process by which most of the pathogenic organisms are eliminated, but not necessary all microorganisms. Spores microorganisms may survive. Disinfection may be of high, intermediate or low level.
The main methods of sterilization and disinfection in dental clinic are physical methods, as heat and irradiation or chemical methods.
I. Heat
A. Boiling water
This method was commonly used in the dental clinics in the past, now it is seldom if ever used. Boiling kills most bacteria within short time. However, bacterial spores survive boiling for a very long time and viruses probably survive indefinitely. For this reason boiling is considered a method for disinfection and not for sterilization.
B. Autoclave (Pressure Steam Sterilizer)
This method of sterilization is the most acceptable method for use in the dental clinics nowadays. It works on the basis of the steam cooker and is an extremely efficient method for sterilization of instruments. The steam is at pressure of about 15 -30 lb/in. This pressure is enough to destroy all organisms and spores.
Chemiclave is another method for sterilization where a chemical is used instead of water. However, this method is not common in dental clinics.
C. Hot-Air Sterilizer (Dry Hot Oven)
It is the most common method used in dental clinics. The disadvantages of this method are:
- In dry condition the organisms are more harder to kill than when they are wet. Also dry heat has very little power of penetration and unless a very high temperatures are used the method is very slow.
- After sterilization the instruments need a considerable time to cool.
- Not suitable for plastic instruments and instruments which have soft solder.
- The heating space is very irregular, the temperature may reach very high degrees in one part and in other part it may not reach the required degree. This is cold "Cool spot".
If this method is used in dental clinics a great care must be taken not to open the oven during the sterilization cycle. Such action, as for adding new instruments, will lower the temperature in the heating space and will mix the dirty and sterile instruments.For proper sterilization the instreuments must remain inside the oven at the required temperature for 120 minutes.
D. Flaming
Some small dental instruments may be sterilized by this method, for example hypodermic needles. However, this method has the disadvantage that the temper of the metal may be spoilt. Irriadioplatinum hypodermic needles can be sterilized by this method. However this is not advisable now as disposable needles are available.
II. Chemical Methods
These methods involve the use of chemical liquid or gaseous compounds.
Liquid Disinfectants
Generally liquids are very unreliable for achieving sterilization. Viruses and both vegetative and sporing bacteria may survive liquid chemical sterilization. It is to be used when other methods of sterilization are unsuitable. The most common used liquid chemical in dental clinics is glutaraldehyde (Cidex). However, this method is used mostly for disinfection as achieving sterilization will take long time (10-12 hours).
The use of effective infection control procedures and universal precautions in dental office and dental laboratory will minimize the risk for cross-infection that could extend to the dentist, dental clinic staff, dental technicians and patients.
UNIVERSAL PRECAUTION FOR INFECTION CONTROL
For surgical procedures in the dental clinics scrub suits and sterile gowns are used. Gowns must be changed after each patient
The term universal precautions refers to a method of infection control in which all human blood and certain human body fluids, saliva in dentistry, are treated as if known to be infectious to human immune deficiency syndrome (HIV) and hepatitis B (HBV) and other bloodborne pathogens. Universal precautions means that the same infection control procedures are used for all patients.
I- Vaccination
DHCWs are at greater risk than the general population of acquiring hepatitis B through contact with the patients. For this reason all dentists and their staffs, having patient contact, should be vaccinated against hepatitis B.
II. Protection and Barrier Technique - A. Gloves
The dentist is most likely to contact blood with his hands. When the skin of the hands is intact it provides good protection from microorganisms that may be in blood. However, in many instances there may be a small unapparent breaks in the skin of the hands. Wearing gloves will provide an extra barrier against the entry of the microorganisms through any break in the skin. Gloves should be used whenever the dentist put his hands in any patients mouth or touch instruments, equipments or surfaces that may be contaminated with blood or saliva of the patient. A new pair of gloves is used for every patient. Instruction for using gloves are listed in table 2.
Three types of gloves are available, these are:
- Examination disposable gloves: Used for procedures involving contact with the oral mucous membrane.
- Sterile disposable gloves: Used when sterility is essential as when performing surgical procedures. Generally this type of gloves is to be used whenever a procedure that involve a break in the mucous membrane of the oral cavity is performed.
- General purpose utility gloves: Used for cleaning instruments, equipments and contaminated surfaces. Rubber household gloves are suitable and can be decontaminated and reused.
Table 2. Instructions for using gloves
- Wash hands before wearing gloves and never wash hands while wearing the gloves.
- Never reuse surgical or examination gloves. Washing these gloves cause wicking which increases the flow of liquids through undetected holes in the gloves.
- If the gloves are cut or punctured remove them immediately and dispose them properly then wash hands again and put on a new pair of gloves.
- When treatment is finished discard the gloves and wash hands again.
B- Face Protection
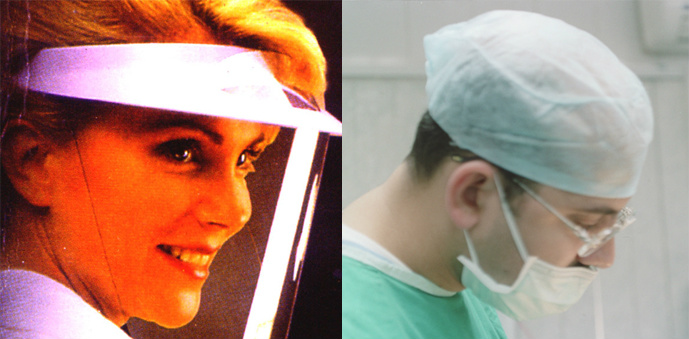
Chin length plastic face shield that protect the eyes, the nose and the mouth from spatter must be used whenever blood or oral fluids contaminated with blood may be spattered, for example during using airrotors.
When face shield is not available eye glasses and face mask must be used. A new surgical musk must be used for every patient and if the mask becomes wet during the treatment of the patient it must be replaced. The eye glasses are disinfectant between patients.
C. Clothes Protection
Protect your street clothes from contamination by covering them with a gown or coat or wearing a uniform. Change these work clothes at least once daily and more often if they become visibly contaminated with blood
III. Care Of Hands
The hands should be washed before gloving and after removal of gloves using soap and water, in case of performing dental examination and nonsurgical procedures. Before and after performing any surgical procedure an antimicrobial agent is used in washing hands.
Skin lesions in the hands of the operator or any personnel of the dental team should be treated and he is not allowing to work before subsidence of these lesions. Finally watches, rings and similar items are not allowed during gloving and working.
Handling Of Sharp Instruments And Needles
Sharp items contaminated with patient’s saliva and blood should be considered as potentially infectious and handled with care. The following should be considered:
- Do not try to recap the needle of the cartilage syringe, by its plastic cover, using your two hands. Use one hand scope technique, table technique or a mechanical device designed for this purpose. The needle should be recovered before removal from the syringe.
- Used needles, scalpels, disposable syringes and similar sharp items should be discarded in a puncture resistance container.
IV. Disinfection And Sterilization Of Instruments
Cleaning, disinfection and sterilization are all decontamination processes. These processes differ in the number of and type of microorganisms killed. Cleaning is the basic first step for all decontamination. By cleaning debris are removed and the number of micoorganisms present are reduced. You always need to clean before disinfect or sterilize.
Disinfection is a process that kills disease causing organisms, but not necessary all microorganisms. There are three levels of disinfection, low, intermediate and high.
- Low level disinfection: Is the least effective disinfection process. It dose not kill bacterial spores or mycobacterium tuberculosis.
- Intermediate level disinfection: Is a disinfection process that dose kill mycobacterium tuberculosis but not bacterial spores.
- High level disinfection: Is a disinfection process that kill mycobacterium tuberculosis and some, but not all, bacterial spores. This process also kills fungi and viruses.
Sterilization, on the other hand, is the process that kills all microbial life, including bacterial spores, which is the most difficult form of microorganisms to kill.
Choice of the decontamination method
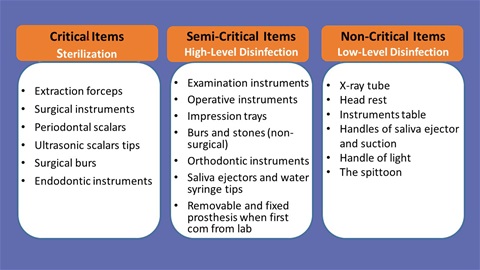
The choice of how to decontaminate an instrument should be based on how it will be used. Accordingly, dental instruments are divided into three groups regarding the level of decontamination required. These are:
- Critical instruments: Are those instruments that will come in contact with bone or penetrate tissue. Forceps, scalpels and scalers are examples for critical instruments. These instruments must be sterilized. Heat sterilization is preferable.
- Semicritical instruments: These are instruments that will touch mucous membrane but will not penetrate the soft tissue. Example of this group is mirrors, amalgam condensers and prosthetic impression trays. These instruments should be heat sterilized or if they will be damaged by heat, use high level disinfection.
- Noncritical Instruments: Are those instruments and environmental surfaces that will come in contact only with the intact skin of the patient. An intermediate or low level disinfection is used for these instruments and equipments.
Sterilization of handpiece
It is essential to sterilize the handpiece between patients. Use handpiece with antiretraction valve (one way valve) to prevent aspiration of the patient’s material into the handpiece and then expelling it to another patient. The handpiece should be autoclaved at 135oC for 15 - 20 minutes between patients. The following should be considered:
- After each patient allow the handpiece to work for 20-30 seconds to expel water and air. This will help to remove any contaminated material.
- After removal from the unite the handpiece is cleaned, lubricated and warped before placing in the autoclave.
Scaler tips and air/water syringe tip
Scalers tips should be autclaved between patients while air/water syringe tip should receive a high level disinfection between patients. A disposable plastic cover can be used for the air/water syringe tips.
Dental laboratory items
Items such as impressions, casts, prosthetic devices and restorations that have been in the patient’s mouth should receive an intermediate level disinfection before sending to the dental lab. The same should be done after manipulation of these items in the dental lab and before placing it in the patient’s mouth. The stability of the material during the disinfection process should be confirmed by the manufacture.
V- Cleaning and disinfection of the dental unite and environmental surfaces
The purpose of this procedure is to remove patient’s material that is possibly contaminating the dental unite and environmental surfaces. This should be done between patients and at the end of the working day. The following methods can be used:
- Disposable towels are used to cover the head rest.
- Aluminum foils or plastic covers are used to cover the light handles, control buttons, X-ray handle, tube and control buttons, as well as handles of saliva ejectors and suction.
- A chemical germicide spray is used to spray the dental chair and the pratice table. An inexpensive methods is the use of fresh solution of sodium hypocholorid (1/4 cup to 1 gallon of water) by swaping the surfavces. This method will give an intermediate level of disinfection.
- A germicide powder is used to disinfect the tubes of saliva ejector and suctions.